From 'goo' to 'go': baby's language development

From "goo" to "go", language development can be both a subject of fascinating conversation and a topic of concern, as Dr Anne Tait describes.
It’s quite remarkable to think that babies are born with crying as their only form of vocalisation, yet within a relatively short amount of time they'll be chatting with you about the colour of the sky, the weather, the bedtime story, the menu...
As with other aspects of a child’s development, when it comes to communication, a lot goes on within a short space of time. During the first three years of life, there is an exponential increase in brain cells. These cells are rapidly forming connections with each other, which is fundamental to the progression from crying to conversation.
Development is a complex interaction between biology and environment. A baby’s brain develops based on the experiences it is exposed to. Babies need their primary caregivers to be in tune with and responsive to their needs, and emotionally connected. This is the foundation for ongoing development – language development in particular. Right from birth it is important that children are exposed to a language-rich environment through interaction with their family to help build their communication skills. If a baby’s brain is not exposed to lots of language coming from the caregivers they love, then it is hard for the brain to build those skills. Communication is a two-way street, with the baby and caregiver communicating back and forth through eye contact, smiling, cooing, babbling and talking. This is the basis for normal language development in neurotypical children.
Straight talking
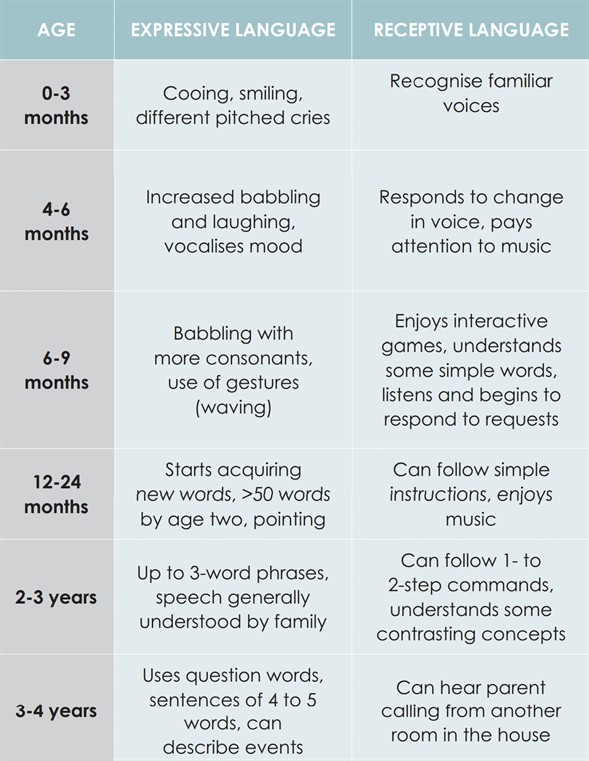
Typically it's good to have an understanding of what ‘normal’ is, to help determine when things are not progressing as expected. Language development involves expressive (spoken) and receptive (understood) language. This table shows normal, but significant, milestones. The timings are approximate.
Talking to the doctor
As with gross and fine motor development, language is not a smooth trajectory and there can be some fits and starts, but the overall progression is forward. Once a child has a 50-word vocabulary, there is a rapid exponential increase in their language skills.
Red flags
The following ‘red flags' trigger the need for more in-depth assessment:
Why the delay?
Thirteen to eighteen percent of 18-36 month olds have some expressive language delay, with 50% of these still having language difficulties by four years of age. Difficulties with language may affect schooling and behaviour later on so early detection and intervention is key. The causes of language delay are many and varied, but some typical diagnoses I see in my clinic include:
Hearing impairment
For any child with language development concerns, it is vital that their ears are examined and their hearing checked by an audiologist. If a child has chronic glue ear, and/or other forms of hearing impairment, this will greatly affect their ability to learn language. However, it is important to note that their non-verbal language should still be normal, even with hearing impairment.
Isolated expressive language delay
This is where children have normal understanding of language and non-verbal communication, normal play, and the rest of their development and examination is normal, but they have a delay in their spoken language. This is what we call a diagnosis of exclusion, meaning that other causes need to be excluded first. This may be due to an underlying language disorder, or not being exposed to enough child-directed language in their environment. For some children, the difference between being in a low socio-economic group as opposed to a high one can be the exposure of around 62,000 words compared to 215,000 words within one week alone – which can later equate to a difference of up to 30 million words by three years of age. This difference can be apparent from as young as 18 months of age, according to a recent Stanford study by Anne Fernald et al. This can lead to some children being up to two years behind their five-year-old peers when they start school.
It is important to know that children learn language from real humans, not the electronic ones. As previously stated, language is not just about talking, but social interaction, love, shared bonds and non-verbal communication, which a child cannot get from electronic devices – even the ones that talk.
Specific language impairment
These are most likely due to a biologically-based neuro-developmental disorder, rather than lack of exposure to language. This diagnosis is made by a speech language therapist using various assessment tools. There are a number of different terms for these conditions, and ‘specific language impairment’ is an umbrella term. Some children get a diagnosis of oromotor dyspraxia, where they have difficulty with the motor movements used for speech. Usually this presents with pronunciation difficulties rather than delay.
Learning difficulties, intellectual disability and genetic syndromes
These learning delays can manifest initially as language delay, although sometimes won’t be apparent till some years down the track. There may be difficulties with gross and/or fine motor development, but not always. Generally speaking, the learning difficulties become apparent in school. There are many syndromes that can present with delayed language development, and these are usually associated with specific facial features, hence assessment by a paediatrician is needed to actively consider these possibilities.
Autistic spectrum disorder (ASD)
This is the main diagnostic category paediatricians are actively screening for, apart from hearing impairment. ASD is a developmental disorder where a child’s communication skills, social interaction and behaviour differ significantly from neurotypical children. This is because of a presumed underlying complex genetic cause affecting early brain development in the embryonic period. It is not due to failure to bond or to speak to the baby early on. ASD is something parents today are more aware of than previous generations and is really a whole topic in itself. It can first present with language delay, but enquiry by an experienced practitioner reveals impairments in social interaction which might not be obvious to others, especially in very young children. When ASD is suspected, there may be a need to do a specific play assessment and observation in early childhood education centres, if the child attends one. The diagnosis of ASD should be made by an experienced professional, who then can refer the child and their family to specialist services for treatment.

AS FEATURED IN ISSUE 37 OF OHbaby! MAGAZINE. CHECK OUT OTHER ARTICLES IN THIS ISSUE BELOW