Having a c-section? Here's what you can expect
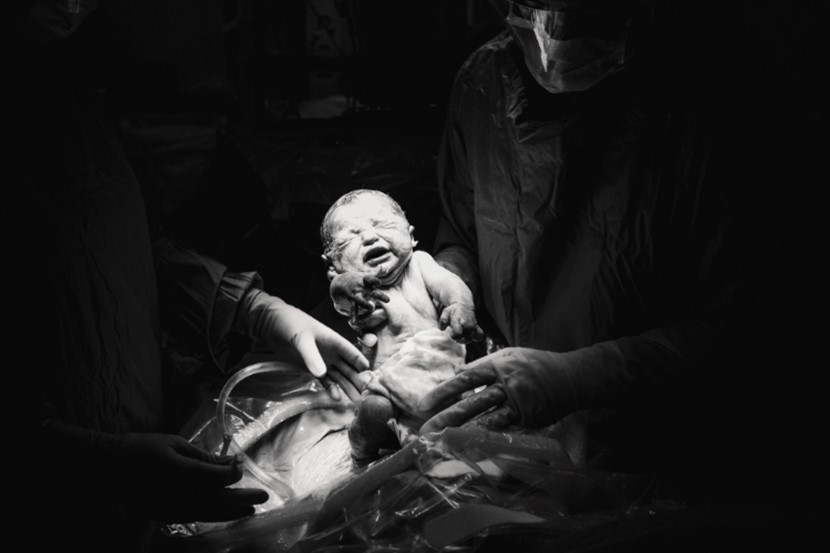
C-sections are a miracle of modern medicine. Obstetrician Dr Nick Walker walks us through this awe-inspiring surgical procedure, so you know what to expect!
You have come at last to the end of your pregnancy, and today will be your new baby’s birthday. Amongst all the planning and preparation, one very major question still remains: how will your baby be born? Will it be a vaginal birth or a Caesarean section (C-section)?
Despite all of humanity’s changes, advances and medical progress over the centuries, these are still the only two options for the healthy delivery of a baby to their mother. When you consider all the complexities and intricacies of reproduction, that the mode of birth comes down to a two-way decision seems to somehow oversimplify the process. Nonetheless, with regards to the everyday miracle that is childbirth, this one really is that simple.
Vaginal birth is a more common outcome in New Zealand than C-section, and because it does not necessarily involve anyone other than the mother and baby, it can rightfully be said to occupy the default position for mode of birth. Indeed, until very recently vaginal birth has been the default mode for the entirety of human history. Read on to learn more about the alternative...
History of c-sections
C-sections have been performed for many hundreds of years across all societies, according to historical records. Up until the early 1900s the procedure is mainly thought to have been done to fulfil religious or legal requirements (to separate a deceased pregnant women from her foetus), without anybody ever imagining that it could possibly confer any benefit to the survival, let alone the health, of a mother. Prior to the advent of modern surgical materials, C-section wounds were left open in a hopeful bid that the mother would survive and eventually heal. Before 1940, the year that penicillin was purified as a drug, the infection complications from C-sections were known to far outweigh any benefit, therefore it was a procedure of ‘last resort’. Following the establishment of modernised ‘women’s hospitals’, and coinciding with the urbanisation of large proportions of the population, many more births took place in a clinical environment. This led to a positive feedback-loop in the progression of the procedure: more C-sections were performed so more was learned about them; they became safer, so more were performed. Better surgical materials and operating environments were brought into play. Even the ability to safely transfuse blood finally became possible. Fast-forward to 2020 and the C-section rate in most developed countries measures between 20-30% of all births. In less than a century, the procedure has evolved from being a desperate ‘last resort’ to the standardised alternative to vaginal birth.

What to expect
C-section is the most common major surgical procedure performed anywhere in the world. The technical aspects of the procedure have been developed and refined to the point where it is considered a safe operation with a very low risk of complications. The vast majority of C-sections begin with a horizontal skin incision low on the front of the abdominal wall, just above the level of the pelvic bone. Next to the skin, another layer, which is tough and fibrous like canvas (known anatomically as the rectus sheath) is also cut horizontally. The good news is that the next layer – the abdominal muscles – does not need to be cut, so you will retain full strength of your ‘abs’ afterwards. The abdominal muscles are gently parted vertically right in the middle (a bit like a pair of curtains) allowing the deeper abdominal cavity to be entered by the surgeon. Next,
a very thin stretchy layer that looks a lot like cling-film (known anatomically as the peritoneum) is opened, beyond which is the wall of the uterus. Finally the uterus is incised and stretched open. Inside is the goal of the surgery: your baby!
Your surgeon is the lucky person who is the first to see, and then touch, your new baby. The tricky part comes next, bringing the baby through each layer that was opened on the way in. As the incisions and thus the exit aperture are small, the baby needs to be born head first or feet first; it is impossible to get them out sideways! To facilitate the birth, the surgeon or their assistant will often exert pressure on your upper abdomen, encouraging the outward movement of the baby in a similar way as to when a mother pushes her baby during vaginal birth.
As baby emerges completely, she or he will become stimulated by the change from the in utero to the ex utero environment and begin to breathe. Mostly these first breaths are manifested by loud and vigorous crying, so everybody in the operating theatre gets to hear your baby’s first noises all at the same time.
Present at every C-section will be a healthcare professional, either a midwife or paediatrician, there to be the second lucky person to see and hold your newborn. The surgeon then passes the baby to them, and if all seems well, the proud new parents will be third in line to see and have contact with their child. At this point the health professionals in the operating theatre all breathe a sigh of relief and enjoy the happy moment, then carry on to complete the operation.
The placenta is delivered following the same route as the baby, then the whole procedure continues in the reverse sequence of how it was begun. Each layer that was opened is now closed with surgical stitches (technically called sutures) of special biologically absorbable thread, as being internal they’re unable to be removed later. Careful attention is paid so that the surgery is clean, and blood loss is kept to a minimum. Antibiotics are always given owing to the absolute certainty they have in reducing post-operative infections. As we started with a skin incision, we finish with skin closure. Common methods include suturing or staples (skin clips) and these are chosen according to patient characteristics and surgeon preferences.
Lastly, a wound dressing is applied and the new family are taken to a post-op recovery area prior to eventual transfer to a postnatal hospital ward.
Emergency or planned?
C-sections can be performed during labour or prior to the onset of labour. The former is commonly called an ‘emergency’ C-section, though I feel this term imparts a sense of immediacy and urgency that is not relevant to most cases. A more preferable term would be ‘unplanned’ or even more precisely ‘intrapartum’, in recognition of the fact that the C-section is being recommended and performed as an alternate to continuing labour and vaginal birth.
The majority of circumstances which occur during labour and which lead to the advice to revert to C-section arise quite slowly and oftentimes many hours may pass in the lead up to the decision. The two most common reasons for performing an intrapartum C-section are when a baby gets stuck or stressed. The cues that indicate foetal stress during labour include the presence of meconium and certain patterns observed on a foetal heart-rate monitor (the monitoring is commonly referred to as a ‘trace’ or CTG). Excepting the rare cases of very sudden and unexpected foetal stress, most often the decision to perform C-section isn’t too urgent.
When a baby is stuck during labour (when labour is ‘not progressing’), by definition there is no rush or urgency either, so there is plenty of time to talk things through with your LMC and the medical team who will perform the C-section.
Elective c-section
C-sections performed prior to labour are most often called ‘elective’. Naturally things are less urgent though still very exciting! The exact sequence of events and personnel involved vary from hospital to hospital, but the general principles of the operation are identical to those of an intrapartum C-section.
Common reasons for performing elective C-sections include foetal breech presentation, multiple pregnancy, issues with the placental position and ‘repeat’ C-sections in cases where a woman’s previous baby or babies were born by the procedure. Occasionally it’s considered when a previous vaginal birth was especially difficult or traumatic, reflecting the fact that there are only two options when it comes to delivery, and a C-section will in this instance seek to provide a better outcome for the mother.
More recently, the procedure is also being considered by some women simply as a preferred alternative to labour and vaginal delivery. The reasons behind such a decision will be varied and specific to a woman’s circumstances, but there’s no doubt that it is again a reflection of both the dichotomous choice of birth and the current safety and surety of C-sections. More widely, it perhaps reflects women’s increasing choices when it comes to their reproductive health.
Unplanned c-section
The majority of C-section births remain urgent and unplanned. The journey towards successful vaginal birth may be diverted at any stage towards the alternative (that is C-section) and I believe all expectant parents should psychologically prepare for this possibility. In the New Zealand health service, the ability to access safe surgery during labour is an underlying keystone of our admirable and excellent perinatal outcomes for mothers and their babies.

When a C-section is done well at the right time, birth retains its status as a miracle – albeit with help from professionally trained ‘miracle assisters’! Some women may feel disappointed, frustrated or even guilty when their birth is by C-section. Often this is based on having worked hard to achieve vaginal birth or conversely, believing they did not work hard enough! When a C-section happens, it’s really important for a woman to understand exactly why it was necessary. With good communication from the hospital team, I believe it’s usually possible to minimise these somewhat negative feelings, a vital step in the now ongoing reality of being a new parent and focussing on Baby and recovery.
Your recovery
Recovery from a C-section is usually straightforward and is perhaps best summed up by this phrase that I hear from many of my own patients: “Not as bad as I thought it would be”. With modern surgical materials and good pain relief, you’ll be encouraged back into normal activities as soon as possible. There’s a common myth that driving a car is not allowed for six weeks afterwards. I suspect this dated back to the days before cars were equipped with power steering and automatic transmission! In the modern scenario, most surgeons might ask you to avoid driving for just two to three weeks.
Unlike every other hospital operation, your C-section has now gifted you a wonderful distraction and motivation to get up and go: your beautiful new baby. Breastfeeding is your new challenge, and you should expect no additional hindrance or handicap in achieving this goal just because you delivered by C-section. The medications you’ll receive are safe and compatible with breastfeeding. Successful lactation relies upon placental hormones declining postpartum (which is why lactation doesn’t initiate whilst still pregnant!) and will happen regardless of the birth method or whether or not labour occurred. Therefore, as long as your baby is latching and suckling well, it’s very important to remain confident that breastfeeding ought to establish as usual.
Finally, although it’s tempting to advise against mundane housework and to recommend lots of pampering if you birth by C-section, of course all new mums should be treated especially well – no matter what!
Dr Nick Walker is a specialist obstetrician working in public practice at National Women’s Hospital and private practice in Auckland. He divides his time between these roles and helping his wife in caring for their four young children.
Top photo: Dr Morgan Edwards, c-section birth

AS FEATURED IN ISSUE 51 OF OHbaby! MAGAZINE. CHECK OUT OTHER ARTICLES IN THIS ISSUE BELOW


















