Birthing: most common pain relief options

Dr Morgan Edwards explains the most common pain relief options available during labour and childbirth.
Women have been using different coping strategies for pain in childbirth for as long as humans have existed! Interestingly, research suggests the more conversations women have about labour and birth, the more empowered they’ll be when the time actually comes.
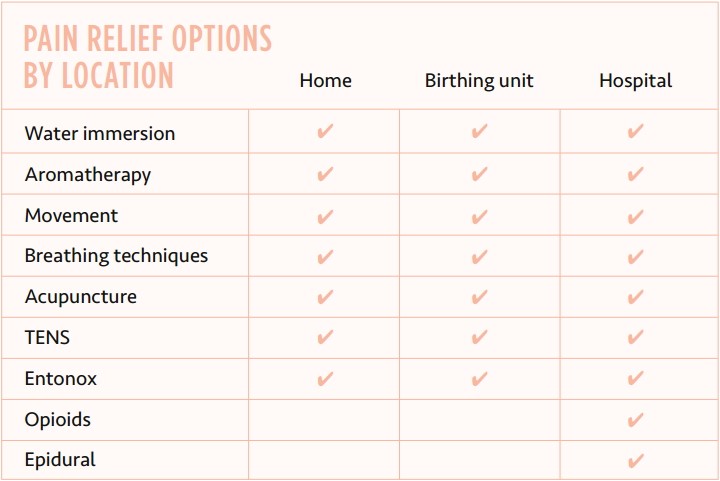
The options to help cope with labour pain vary depending on where you’re birthing. While some are restricted to hospitals only, many are available wherever you choose to birth. Let’s start by looking at some of the more common drug-free pain relief choices.
DRUG-FREE PAIN RELIEF CHILDBIRTH EDUCATION
This may seem like a strange one to begin with as it’s not for during labour. However, we know that attending antenatal classes, either in person or remotely, is strongly associated with a positive birth outcome. These classes, which are usually offered free through your local health board, talk about pregnancy, labour and birth, breastfeeding and caring for your newborn. They’re a good chance to ask questions and can also help you form a support group of other local parents with whom you can talk through options and choices. Research shows these sorts of informal talks can help you find your own style and preferences. Also, many women find the friends made in their antenatal class become a helpful support group after baby is born.
RELAXATION & BREATHING
Relaxation and breathing techniques can be used right from the start of your labour and have been shown to help you relax, to relieve labour pain and to give you an increased feeling of control.
During your contractions you can do rhythmic breathing, releasing tension as you exhale. There are no known drawbacks of using this technique, and it’s something you can also practise during pregnancy. Some studies have shown that relaxation techniques, such as yoga, can also reduce labour pain intensity as well as increase labour satisfaction.
BIRTH ENVIRONMENT
Making sure you have a comfortable place to give birth can be very helpful. Ideally somewhere private and relaxing with plenty of room to rest, bathe and walk around. Many birthing centres and delivery units encourage you to visit when you’re pregnant so you feel more comfortable there when the time comes. You can usually bring some personal items from home, such as an oil diffuser or your favourite pillows, to help create a relaxing home-like environment in your birthing room.
MIDWIFE SUPPORT
The presence of a trusted, nurturing support person, such as your midwife, is known to be the most important factor when it comes to having a positive birth experience. We’re so fortunate in New Zealand to have the phenomenal Lead Maternity Carer midwife care model. A midwife gives you emotional support, guidance and information throughout your pregnancy and labour. They can also help during labour with things like massage, and be an advocate for you.

MATERNAL MOVEMENT AND POSITIONING
Moving and changing positions to help control labour pain is one of the oldest coping strategies known. As well as helping provide comfort, caregivers can help by suggesting certain positions to aid labour progress or to correct any issues with you or your baby. We know that especially early in labour, upright and walking positions can help make things progress faster and reduce your chance of other intervention, and usually aren’t associated with any harm.
BIRTH BALL
Many women find a birth ball allows freer movement and helps give a sense of control. By using a birth ball in the sitting position you can create a non-painful pressure on the perineum, which may block some pain messages and help with relief.
WATER IMMERSION
You might have heard about water births, where women spend some or all of their labour immersed in water. Lots of research has shown that labouring in water deep enough to cover your whole belly increases relaxation and decreases the need for other kinds of pain relief.
Lots of women find water brings relief at different stages of their labour. Many delivery units have birthing pools so ask your midwife about what’s available at your local delivery unit.
TOUCH AND MASSAGE
Massage can be used for pain relief in your labour, and can be useful for reducing anxiety and increasing emotional wellbeing. Touch can be a very powerful way to communicate positive messages of reassurance and love.
ACUPUNCTURE AND ACUPRESSURE
Acupuncture and acupressure have been shown to reduce the need for pain relief drugs, and reduce the use of interventions in the birthing process. Research also shows that women find acupuncture helpful in labour. You’ll need to talk to a professional about whether this is an option where you are planning to birth.
HYPNOSIS
Hypnosis involves a deep state of relaxation with an alert mind. There are multiple techniques that can be learnt before you go into labour. Many women find hypnosis gives them an increased sense of control. Your midwife can usually help you find more information about hypnosis and how you could use it for your labour.
AROMATHERAPY
Aromatherapy is the use of highly concentrated essential oils or essences distilled from plants, and it can be used to soothe and reduce fear, anxiety and pain. You can talk to a professional, such as a naturopath, about which oils are safe and effective in labour and how to use them.
Many birthing units won’t allow naked flames but an electric aromatherapy burner can often be used instead.
TENS MACHINE
TENS (transcutaneous electrical nerve stimulation) is a straightforward and safe type of drug-free pain relief. TENS works by passing a very small electric current across your skin, which can help mask pain impulses and provide relief. You place small, soft electrode pads on your lower back, and control the intensity of the impulses. As your labour progresses, you can increase the intensity as you need.
You can arrange to hire a TENS machine through your local pharmacy, your midwife or online, and once you’re in labour, start using it whenever you feel it helps.
MEDICAL PAIN RELIEF
In addition to drug-free pain-coping strategies, there are also a range of medications available for labour and birth. The most commonly used medication is Entonox, also fondly known as ‘gas’.
ENTONOX
Where it’s available, you can choose to use Entonox at any time in your labour. You breathe it in through a hand-held mouthpiece. The idea is that you start using it when you feel a contraction coming on and breathe normally through the mouthpiece until the peak of the contraction has passed. Some women find Entonox gives enough pain relief for the whole of their labour, others may choose stronger pain relief later on. Entonox is safe to use for your labour, and is safe for your baby, with no lasting effects.
OPIOIDS
Opioids are strong pain-relieving drugs that all work in a similar way to each other. They’re usually only available at hospital birthing units. The opioids commonly used on labour wards in New Zealand include morphine, pethidine and fentanyl. Some labour wards also use another opioid called remifentanil.
Your midwife usually gives opioids by injecting them into a large muscle in your arm or leg, but they can also go through a drip into your vein. Depending on the drug used, you can start to feel the effects in just a few minutes, or they can take up to half an hour to work. The pain relief they give can last from a few minutes, to several hours.
In some labour wards opioids can also be given regularly into your vein, using a pump that you control yourself with a button. This pump is called a PCA (patient controlled analgesia). PCAs are sometimes available if it isn’t possible for you to have an epidural. If you do have a PCA, you’re able to give yourself small doses when you feel you need them. The pump is set up so that you can only give yourself a safe amount. Sometimes women are worried that taking opioids might make them or their baby addicted, but we know that using opioids for a short time during your labour is safe and is unlikely to lead to any type of addiction later in your life or your baby’s life.
Opioids can have some effects on your baby – they may be drowsy and slower to take their first breath. If this happens, the health professionals looking after you will make sure your baby is safe. However, with most opioids, the effect on your baby is usually very small.

EPIDURALS
Epidurals are available only in hospital-based birthing units, and can only be placed by anaesthetic doctors. They work by temporarily blocking pain messages from the lower half of the body.
Epidurals require more preparation than other methods of pain relief and take on average 30 minutes to get you comfortable. They involve placing a small plastic catheter into the epidural space in your back. Once it’s in place, pain-killing drugs can be injected – either by a pump or topped up by hand. In some hospitals you can press a button when you need more pain relief. Once it’s working, an epidural can be kept going until your baby is born.
As for any medical intervention, there are some potential risks associated with epidural insertion:
✔ More commonly you can experience some degree of leg weakness and numbness, but most women find they’re able to push. You may not be able to feel when you need to go to the bathroom, and will likely need a tube placed in your bladder once the epidural is working.
✔ Some epidurals don’t work completely effectively right away and need some adjusting to achieve the best amount of pain relief. Occasionally an epidural will need to be reinserted.
✔ Less common side effects include developing a headache that could last several days. Normally this can be picked up early and treated.
✔ More serious side effects, such as nerve injury and infection, are extremely rare and the risk of serious permanent harm is low.
✔ You may be concerned that an epidural could lead to long-term back pain, however we know there is no increased risk of this.
✔ Epidurals may make your labour last slightly longer, and you may need a drip to make your contractions come more frequently. They may also be associated with a greater chance of needing forceps or ventouse for your birth. Having an epidural does not make it more likely that you’ll need a Caesarean section. If your baby does need to be delivered via C-section, it’s usually very easy to boost your epidural so it can be used as your anaesthetic, and you can stay awake to see your baby being born.
About 25% of New Zealand women choose to have an epidural in their labour, with first-time mothers being induced the most likely to choose one.
PERSONAL PREFERENCE
Choosing pain relief is very personal. Research shows that using one or more of these methods in your labour may help to reduce stress and increase your natural hormone levels, including oxytocin, prolactin and beta-endorphins. These hormones naturally peak in late labour contributing to effective labour progress and providing natural analgesia (pain relief). Research also shows that increased levels of these hormones may promote contractions, reduce haemorrhage risk and support successful breastfeeding.
You can choose one or more of the above approaches at any stage of your labour, and practise many in advance too. Talk to your midwife about any questions you have and about finding additional information on any options that interest you, and what’s available at your local birthing unit.
Dr Morgan Edwards is a consultant anaesthetist at Auckland’s North Shore Hospital. Morgan is also a mum, and she’s passionate about empowering Kiwi women to have positive birthing experiences by providing them with good information on all the pain relief options available to them. Visit her website yourlabouryourway.co.nz.

