What to expect during a c-section
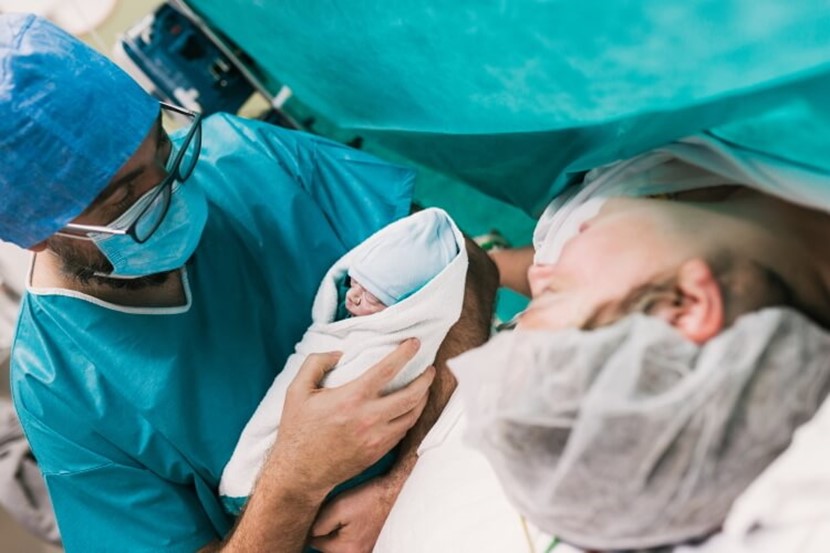
The maternity team attending a C-section birth consists of a midwife, theatre nurses, anaesthetist, anaesthesia technician, obstetrician, paediatrics nurse or doctor, and your support person. That means a lot of people in a large bright operating theatre. Check with your hospital for their policy on how many support people can stay with you during the operation. All members of the team should introduce themselves to you before the procedure begins. The team should also be following the Surgical Safety Checklist developed by the World Health Organization – ask if your hospital participates in this internationally recognised initiative.
At the start of the operation, you should receive a single dose of intravenous antibiotics to reduce the risk of developing an infection after the operation. This is safe for your baby.
The anaesthetist meets you before your operation to discuss the choice of anaesthetic and answer questions. Most C-sections are done under regional anaesthesia, meaning you are awake but sensation from the lower body is numbed. This is generally thought to be safer for you than being put to sleep (general anaesthesia), and your baby will be more alert at birth. Another advantage of regional anaesthesia is that you can start bonding with your baby right away, as you can have skin-to-skin contact and breastfeed during the operation if you feel comfortable to do so. Some women, unfortunately, feel drowsy, lightheaded or nauseous as side effects of the anaesthetic. Your midwife or support person should be able to help in this situation and ensure you experience skin-to-skin contact with your baby as soon as you feel better – in the recovery room, for example.
There are three types of regional anaesthesia:
1. A spinal may be used in planned or emergency C-section. The spinal cord and nerves carrying pain sensations from your womb and legs are contained in a bag of fluid inside your backbone. Local anaesthetic and a pain reliever are injected into this space in your back using a very fine needle. A spinal works quickly with a small dose of anaesthetic.
2. An epidural is where a thin plastic tube (or catheter) is put just outside the bag of fluid to inject medication near the nerves. An epidural is often used for pain relief in labour, and can be ‘topped up’ by using a stronger local anaesthetic solution if you need a C-section delivery.
3. A combined spinal-epidural is a combination of the two. The spinal makes you numb quickly and is used for the C-section. The epidural can be used to give more anaesthetic if needed during the operation and to give pain relief afterwards.
Dr Michelle Wise (MD, MSc, FRCSC, FRANZCOG) is an obstetrician and gynaecologist at National Women’s Hospital in Auckland and a senior lecturer in the Department of Obstetrics and Gynaecology, University of Auckland.
Main image: istock

AS FEATURED IN ISSUE 36 OF OHbaby! MAGAZINE. CHECK OUT OTHER ARTICLES IN THIS ISSUE BELOW


















